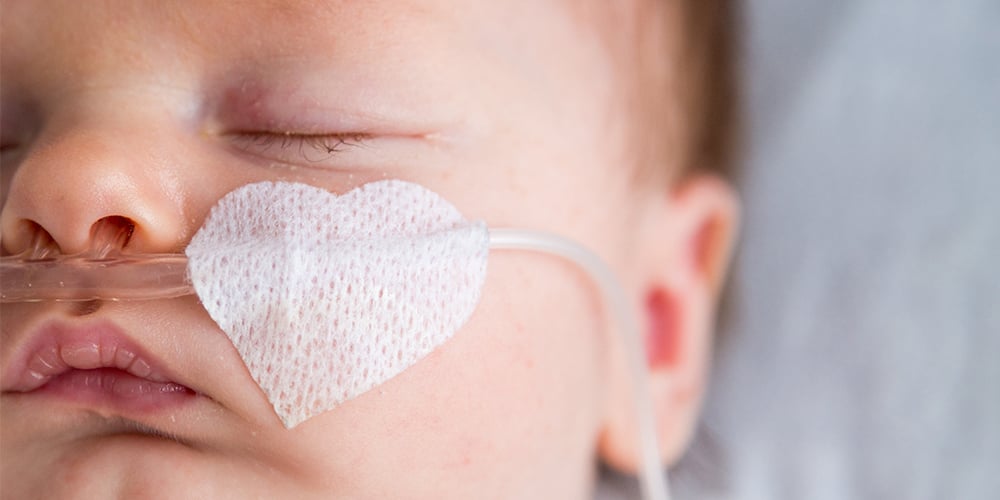
The Challenge of Health Literacy After a NICU Stay
Posted by
Madeline Szabo, RN, BSN on December 21, 2023 at 4:00 PM
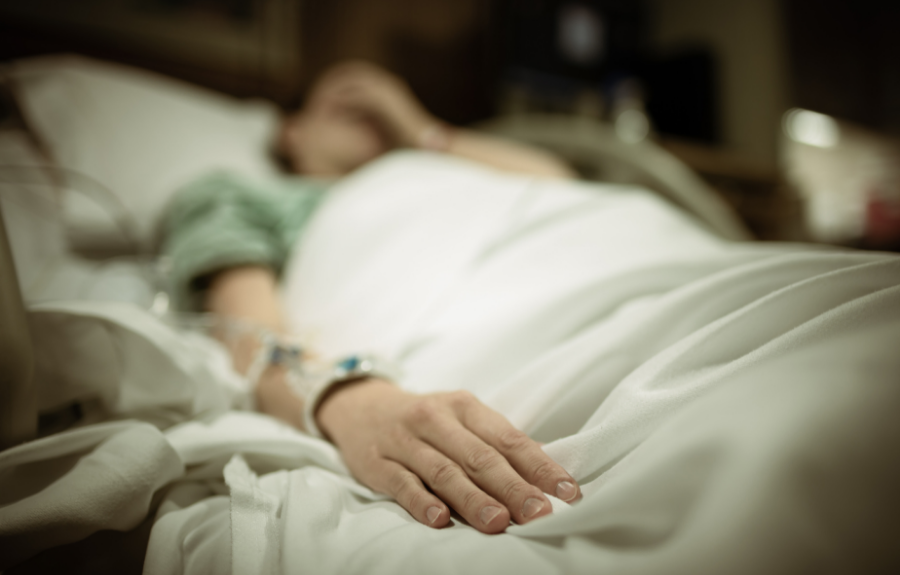
From Birth to Bills: Understanding the Impact of Preterm Births on Financial Well-Being
Posted by
ProgenyHealth on November 8, 2023 at 8:40 AM
Breaking the Cycle: Preventing Neonatal Abstinence Syndrome and Nurturing Healthy Beginnings
Posted by
ProgenyHealth on September 12, 2023 at 2:32 PM
5 Trends Impacting Maternal and Infant Health in 2023
Posted by
ProgenyHealth on February 8, 2023 at 9:00 AM
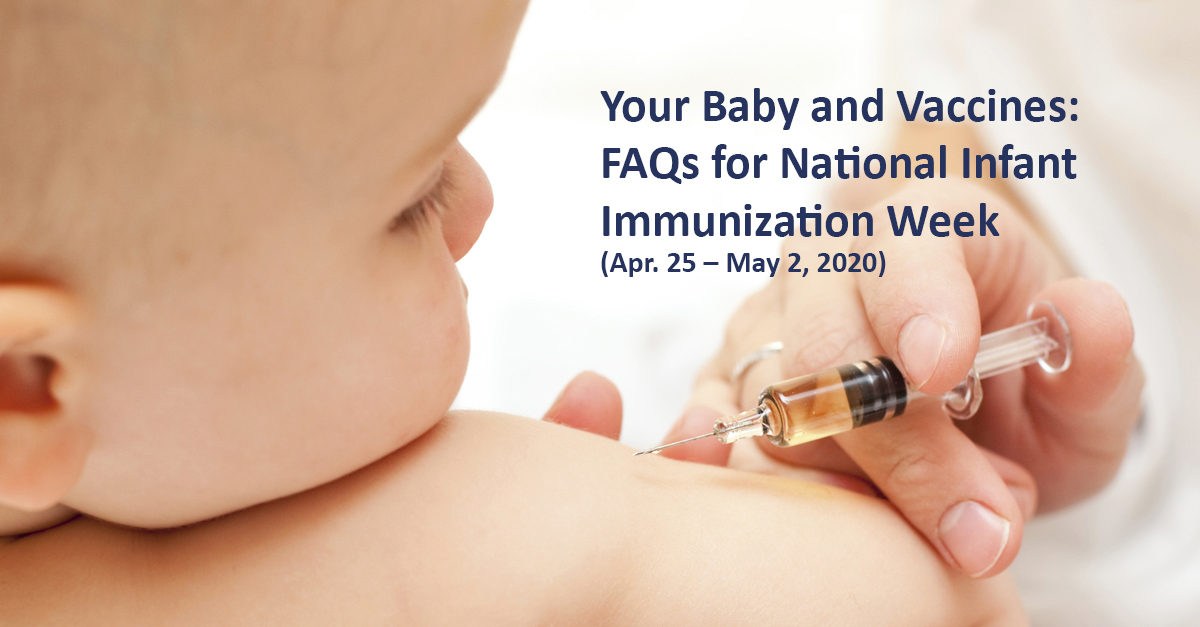
The Continuing Importance of Vaccines for Infants and Children
Posted by
ProgenyHealth on November 28, 2022 at 12:30 AM
Managing the Key Cost Lever for Your Maternal Health Program
Moving the needle on maternal morbidity creates positive downstream effects
Posted by
ProgenyHealth on July 7, 2022 at 8:00 AM
Paying Dividends
How NICU Care Management Frees Up Funding for Major Initiatives
Posted by
ProgenyHealth on May 25, 2022 at 10:00 AM
10 Reasons to Integrate Family Benefits into your Health Plan Package
Posted by
ProgenyHealth on May 10, 2022 at 8:57 AM
Provide a short summary of this article here. This summary will show up on the Blog Listing page.