 Filed Under: NICU
Filed Under: NICUWhat Graduation Day Means to My Family: Love for National Children’s Day

June is the month for honoring graduates – the end of a period of focused educational effort and the beginning of a new stage in a life full of promise. Although commencement ceremonies and family parties will look much different this year, well-deserved recognitions will still happen. But there is a lesser known category of graduates who achieve so much worth celebrating, and they do so years before their first day of school: infants who spend their first days, weeks, or months of life in a neonatal intensive care unit (NICU). I would like to tell you my story, not just as General Counsel and Chief Compliance & Privacy Officer of ProgenyHealth, but as the mom of a NICU graduate.
June 14th is National Child/Children’s Day
A day to cherish, spend time with, and redirect our energy and focus away from modern distractions and toward those that give our lives true meaning. It is also a time to see our children for who they are and help shape who they are becoming through all those unique life experiences. On this day, I am reminded to cherish them for who they are, and to be grateful for all of our experiences as a family.

I have spent the last 9 ½ years of my career focused on managed care, while raising two children whose experiences in this world have already been very different from one another. For my husband, Steve, and I, we generally spend Sundays as a family; quality time with our children: Bryce (age 9) and Quinn (age 6). We have spent plenty of time with them lately, but all too often it has been directing them to do something (homework, reading, Zoom meetings), or decompressing with them after our crazy days of working and schooling at home.
But this National Children’s Day, we want to take a moment and ask our kids: How are you? Are you happy? What are your favorite things to do? Are you enjoying childhood? What are you most looking forward to this summer? And then, listen to the answers; answers from our children who are excited and eager to share their thoughts and feelings on their life and journey.
Bryce was our first child – born a week past his due date at a healthy 8lbs. 8oz., and already strong enough to hold his head upright at birth. I recall holding him for the first time and feeling how wide his shoulders were and being astonished at how solid he already was. Bryce was an easy baby, healthy and strong – breast fed for 13 months, solids at 6 months, and his favorite food is still carrots. He rolled over on time, crawled on time, walked on time, and started talking on cue. “Hi” was his first word. How appropriate, because he has never been shy; he loves talking, making friends, and is a jovial kid who is fun to be around.
It was just after Bryce’s 3rd birthday that Quinn was born. We had just celebrated Bryce’s big day, spending a summer day in downtown Pittsburgh and attending a baseball game. My girlfriends had just thrown me a “Baby Sprinkle” to welcome Quinn, who was due in September. It was like any other hot, humid, July weekend morning – and I was daydreaming about taking a summer beach trip. But Miss Quinn had other plans. It was thirty-three weeks and 5 days into my pregnancy. This is too soon, I thought.
I had just had my regularly scheduled checkup the week before, and everything was normal. After listening to my symptoms, my doctor told me to go to the hospital to get checked out immediately. Steve, Bryce, and I loaded into the car and sped off to the hospital. Little did I know that moment would be the last time we would be home as a family of three. Once I arrived at the hospital, they confirmed that my amniotic sac had torn. I was admitted to the antepartum unit where the doctors took great care to talk with me about what to expect in the days to come, including steroid injections to develop her lungs, a cesarian section because she was breach, and preparations for what would likely be an admission to the neonatal intensive care unit (a concept we were familiar with, as I was working in Medicaid managed care at the time and was involved in many coverage matters involving children who were initially NICU babies). The overwhelming fear set in as we wondered whether she would be a healthy and strong baby, like her brother. That Monday morning, Quinn was born. 4lbs. and 17 inches long, with hypoglycemia and high bilirubin, requiring C-Pap, suffering recurrent episodes of apneas and bradycardias. We learned an entirely new language in those following days and became part of a community I never knew existed – we were now a NICU family.
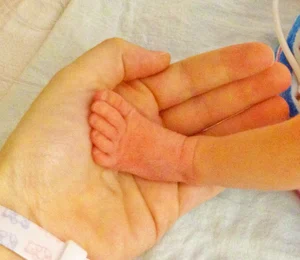
Quinn spent her days in her incubator – a hard, temperature-controlled plastic container with portholes for your hands. I was a working mom on maternity leave and spent my days by her bedside with my hand through the porthole, holding her hand or slowly stroking her eyebrow. A perfect little eyebrow that was smooth and silky, on a perfect little face, with the cutest button of a nose; a nose with a tube coming out of it – a nasal cannula (because she was not developed enough to eat by mouth, she was fed by a syringe via her nasal cannula). There would be no breastfeeding for this baby, and I would come to miss that closeness I had with Bryce. Some days I could not hold her hand because it was wrapped in gauze from the IV in her arm, so I would gaze in wonder at her foot. A foot that was no bigger than my thumb, and five little toes that were the size of lady bugs, that she wiggled when I ran my finger down her foot. Even at 3 days old it was as if she was ticklish.
Every day I would participate in her care plan with the nurses and doctors. We would sit in a circle together in the open part of the NICU floor during rounds. I got a chair in the circle. I would call Steve, who would listen in from work when he was available. And I would wait for those words – what milestones Quinn needed to hit next to be able to come home. First, it was the phototherapy for her bilirubin levels. Next, it was the removal of the IV. Then, it was the removal of the nasal cannula and eating by mouth, without losing weight. Every day we tracked her weight and obsessed over pounds and ounces. I was bedside 8:30am to 5:30pm while Steve was at work and Bryce was at preschool, and then I would call the night shift nurse to see how she had been since I left. On weekends we would spend midday with Quinn, taking turns holding her, and letting proud big brother Bryce spend time with his new baby sister.

It took her 10 days to reach her birthweight of 4lbs again. In the meantime, the apneas (loss of breathing) and bradycardias (slowed heart rate) dominated our days and nights. Each event extended her stay in the NICU and kept us from bringing our baby home. “She will grow out of it,” they would tell us. But we could not stop thinking: what happens if she doesn’t? What happens if she stops breathing and does not start again? In the NICU, there were machines to monitor her breathing and heart rate and provide a stimulus to surprise her into breathing. If that did not work, the nurse would come over and flick her foot or gently stimulate her. But at home, there were no machines or nurses.
Graduation Day for Quinn
After 17 days in the NICU, we brought Quinn home – on a cardiorespiratory monitor (home apnea monitor). Not quite the homecoming we had pictured: our baby in her car seat, propped up and protected by rolled receiving blankets, looking like a doll in her spacious car seat. She had a heart monitor wrapped around her chest with wires coming out of one side, which all lead to a monitor that would shriek if she stopped breathing for too long.
We had been so focused on bringing Quinn home that I am not sure we stopped to realize that once she did come home, all of that care and attention was solely for us to provide. We were anxiously watching every breath, responding out of adrenaline when the monitor howled at 2 am, and once again watching her weight.
My maternity leave ended after 6 weeks and I needed to go back to work. I was lucky enough to be established with a great daycare for Bryce that would accept Quinn, who was still on the monitor. She started daycare 6 weeks after she was born, at only 5lbs., 8oz. I returned to work and spent my days trying to get back into the daily grind of work/life balance. But, how could I focus on my work? We now had a special baby who required extra care, and our life was not necessarily set up to accommodate that. I recall having a call with a case manager from my insurance company, talking in generalities about how things were going, but there was no definitive action taken to provide us with assistance. I had meetings at the hospital to check Quinn’s weight, which was increasing in the smallest of increments. This made me feel like a failure in comparison to Bryce, who gained in leaps and bounds.
It was not until around Thanksgiving that things really changed for us. Quinn got sick, was losing weight, and was diagnosed “failure to thrive.” Those words were scary to us, but we knew it meant we were about to get some help. She qualified for Early Intervention, and with that came weekly and monthly meetings with an occupational therapist to work on Quinn’s nutritional needs – seeing that she didn’t eat a lot in volume, we worked to find the most calorie and nutrient dense foods. We participated in nutritional and occupational therapy for two years and found all sorts of ways to sneak in extra calories to Quinn’s meals so she could continue to gain and grow. It changed a lot of what we did as a family, causing more stress, anxiety, and insecurity. But, luckily, Quinn is a fighter. She fought to roll over at 4 months, fought to stand upright at 10 months, fought to walk by 13 months. And for all she fought with me as I tried to make her first word “ma-ma,” it was “da-da.”

Today, Quinn is an outgoing, precocious, smart little girl. She thrives on social time with friends. At 2 ½ we started her in dance and gymnastics to build her core and flexibility in her hips (she had dysplasia at birth), and by 5 years old she was invited to join the competitive gymnastics team. She says she wants to be a veterinarian, for her love of animals, though she often pronounces it “vegetarian” (hysterical, since her favorite food is cheeseburgers!). She loves dance, gymnastics, art, and singing. For a preemie – a kid who loves doing things early – I should not have been surprised that she was an early reader who is now already reading some of her brother’s books.
As we put her to bed every night, she starts negotiating the next day. “Can I have a playdate? Can we do a firepit and make s’mores? Can I have the iPad when I wake up?” And my response is always: “Let’s talk about it tomorrow.” As I send her off to sleep with a kiss on her forehead, running my fingertips over that perfect little eyebrow that I have adored since the instant she was born, I am in this moment appreciating the journey the four of us have been on with these two completely different and equally amazing little children who have captured my heart.
With this unique perspective, I see so many ways that ProgenyHealth can help babies like Quinn and families like ours across the country, right now. Our team could have ensured I went back to work with confidence that Quinn was getting what she needed on a daily basis. It is why I love what I do here at ProgenyHealth. It is why I believe so strongly in the mission and purpose of our organization. And it is why I know that we are passionately driven by a greater cause.
And so, I do my part to ensure fellow NICU families are provided with the support they need to reach that first and most important graduation day, make their transition home easier, and keep their babies healthy. I want to ensure those nights of bedside chats and forehead kisses endure for so long as our children will let them – cherishing those children, especially on this National Children’s Day.
Elysia Tomlinson is General Counsel and Chief Compliance & Privacy Officer at ProgenyHealth
BLG038






 Prev
Prev